A Guide to Angioedema: Symptoms, Causes, and Associated Risks
Angioedema is sudden swelling that can affect the face, limbs, gut, or airway—and the risks change depending on the cause. This guide explains key angioedema symptoms, what causes angioedema (including allergy, medication-related, and hereditary pathways), and why throat swelling is treated as urgent. You’ll also find practical prevention ideas, comfort-focused strategies for swelling reduction, and a clinician-ready checklist to help clarify triggers and next steps for recurrent episodes.
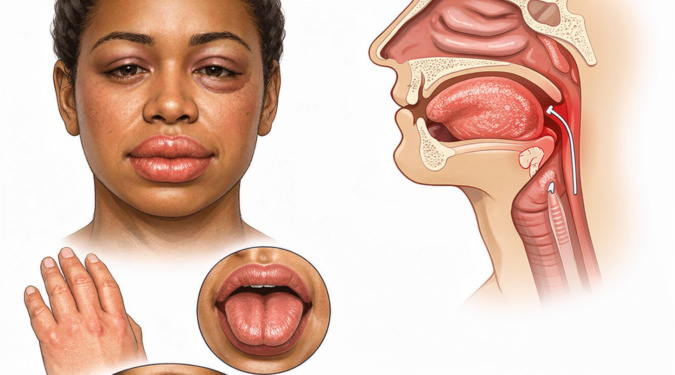
Angioedema can show up fast—swelling that changes your face, hands, or airway in hours, not days. This guide walks through angioedema symptoms, what causes angioedema, and the risks that matter most, including hereditary patterns and when throat swelling becomes an emergency.
What Angioedema Is And Why It Happens
Angioedema is swelling in deeper layers of skin and mucous membranes, often around the eyes, lips, tongue, genitals, or inside the gut. It can be triggered by histamine (commonly allergy-related) or by bradykinin (commonly medication- or hereditary-related). Knowing which pathway is likely helps clinicians choose the right angioedema medication, because common allergy treatments may not work for bradykinin-driven swelling.
Common Symptoms And What They Can Look Like
Typical angioedema symptoms include sudden puffiness, tightness, or a burning/pressure feeling more than itch. Skin may look normal or slightly red, and the swelling can migrate. Many people search for angioedema pictures to compare patterns, but appearance alone can’t confirm the cause—timing, triggers, and response to treatment are often more useful clues.
Airway And Throat Warning Signs
Angioedema throat swelling can feel like a lump in the throat, hoarseness, trouble swallowing, drooling, or noisy breathing (stridor). Any rapidly worsening mouth or throat swelling is treated as urgent because airway narrowing can progress quickly, even if the skin swelling seems mild.
GI And Neurologic-Like Symptoms
Some cases cause crampy abdominal pain, nausea, vomiting, or diarrhea due to bowel wall swelling. People also sometimes report headache, dizziness, or brain-fog during severe episodes; this is sometimes described online as angioedema neurological, but it’s often indirect (stress, low oxygen if breathing is affected, medications, or systemic inflammation) rather than swelling in the brain itself.
What Causes Angioedema
When people ask what causes angioedema, the answer is usually one of a few buckets: allergic reactions (foods, insect stings, latex), infections, physical triggers (pressure, temperature change), autoimmune conditions, medication effects, or inherited complement problems. Episodes may occur with hives in histamine-driven forms, but hereditary angioedema and many medication-related cases often occur without hives.
Recurrent And Hereditary Patterns To Know
Recurrent angioedema is often defined by repeated episodes without a clear one-time exposure. A family history of similar swelling, onset in childhood/teens, recurring belly attacks, and poor response to antihistamines can raise suspicion for hereditary angioedema (HAE), which involves C1 inhibitor pathway dysfunction. Even without family history, new mutations can occur, so the overall pattern matters.
Medication-Related Triggers And Treatment Options
Several drugs can be associated with swelling; the most recognized category is ACE inhibitors, which can provoke bradykinin-mediated angioedema even after long-term use. Treatment depends on severity and suspected mechanism. Histamine-driven cases are often treated with antihistamines, corticosteroids, and sometimes epinephrine for anaphylaxis. Bradykinin-driven cases may require targeted therapies (such as C1 inhibitor concentrate, icatibant, or ecallantide) in appropriate clinical settings.
Associated Risks And When To Seek Emergency Care
The biggest immediate risk is airway compromise. Another risk is misclassification—assuming “all swelling is allergy” can delay effective care for bradykinin-driven episodes. Repeated attacks can also cause anxiety and missed work or school, and abdominal attacks can lead to unnecessary imaging or procedures if angioedema isn’t considered.
Practical Steps For Prevention And Swelling Reduction
Angioedema prevention focuses on trigger identification and a clear action plan, especially for those with repeated episodes. For how to reduce angioedema swelling during a flare, clinicians often emphasize early recognition, avoiding known triggers, and using the prescribed rescue plan quickly; cool compresses and resting upright may help comfort, but airway symptoms always outweigh home measures.
A Simple Angioedema Checklist For Your Next Appointment
- Where the swelling starts (lips, eyes, tongue, hands, genitals, abdomen) and how fast it spreads
- Whether hives/itching occur, and if antihistamines helped
- Possible triggers in the prior 24 hours (new foods, infections, stings, pressure, temperature changes)
- All medications and recent changes, including blood pressure drugs
- Family history of similar swelling or unexplained abdominal attacks
- Any voice change, swallowing trouble, or breathing symptoms
Angioedema Guidelines And Follow-Up Planning
Many angioedema guidelines emphasize stratifying episodes by airway risk, identifying histamine vs bradykinin features, reviewing medication triggers, and considering specialist evaluation (allergy/immunology) for recurrent or unexplained cases. A written plan—what to take, when to seek urgent care, and what to avoid—can reduce delays during future episodes.
FAQs
Can Angioedema Happen Without Hives?
Yes. Bradykinin-driven angioedema (including ACE inhibitor–related and hereditary forms) commonly presents without hives, which is one reason it can be mistaken for “mystery swelling.”
How Long Do Episodes Usually Last?
Histamine-driven swelling may improve within hours to a day with appropriate treatment. Bradykinin-driven swelling often lasts longer—commonly one to three days—though duration varies by person and treatment timing.
Is It Safe To Wait And See If Throat Symptoms Improve?
Any worsening mouth or throat symptoms are treated as urgent because airway swelling can progress unpredictably. Emergency teams prioritize airway assessment and cause-appropriate therapy.
What If Episodes Keep Coming Back?
For recurrent angioedema, documenting patterns and reviewing medications is a common first step, followed by targeted lab evaluation when hereditary or complement-related causes are suspected.
Conclusion
Angioedema is more than “simple puffiness”: its symptoms, causes, and associated risks vary widely depending on whether the trigger is histamine, bradykinin, medication-related, or hereditary. Recognizing throat warning signs, tracking recurrent episodes, and aligning care with established guidelines can make future events safer and less confusing.
Disclaimer: The information provided in this article is for educational and informational purposes only. It does not constitute professional advice. Readers should conduct their own research and consult with qualified professionals before making any decisions.